Understanding its Anatomy and Function
Introduction
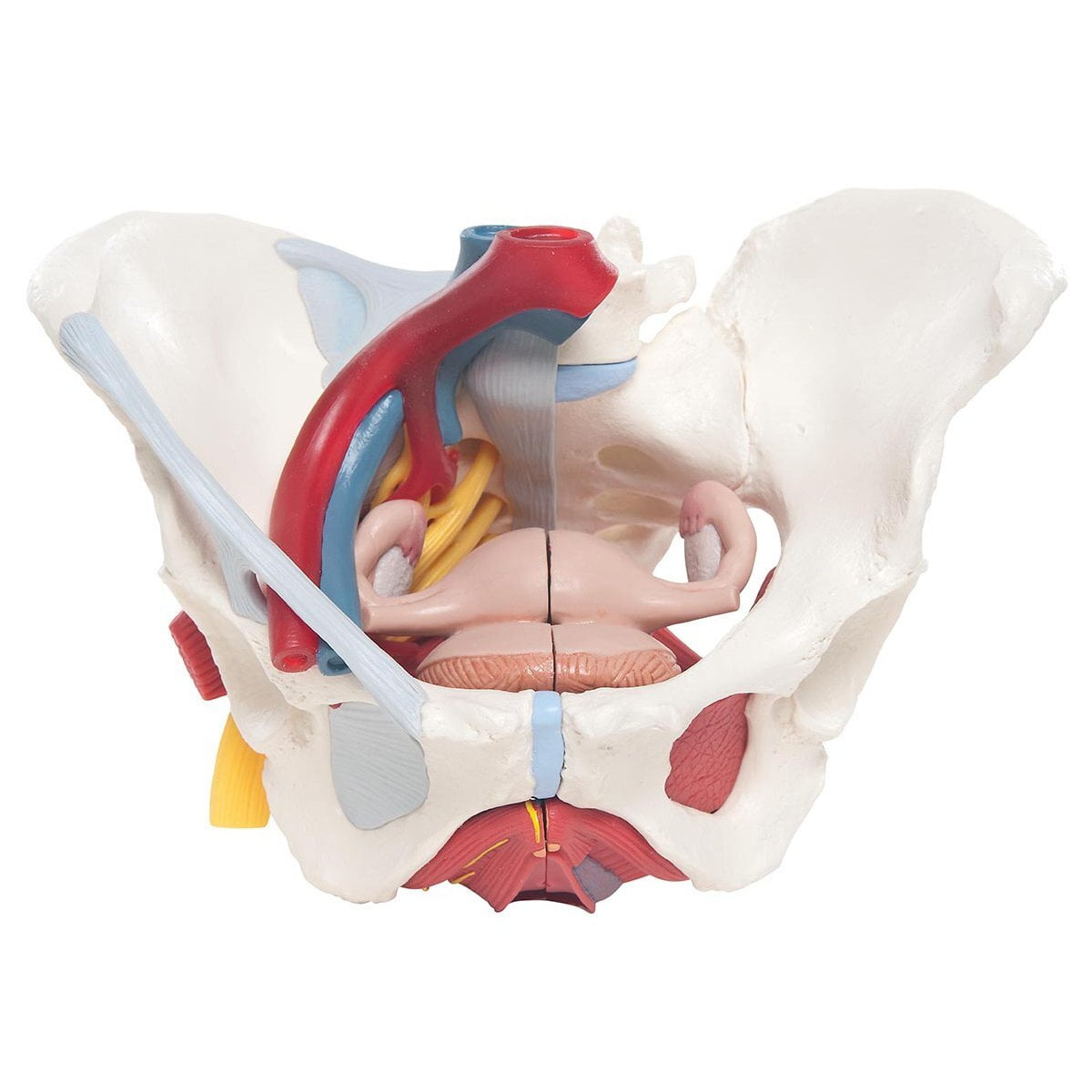
The female pelvic floor is a complex structure that plays a crucial role in supporting the pelvic organs, maintaining continence, and ensuring sexual function. Understanding its anatomy is essential for healthcare professionals and individuals seeking to maintain optimal pelvic floor health. In this article, we will explore the major muscles, nerves, blood supply, and bones that comprise the female pelvic floor.
I. Bones of the Female Pelvic Floor:
The female pelvic floor is formed by several bones that provide a sturdy foundation for the pelvic organs and muscles. These bones include:
- Sacrum: The sacrum is a triangular bone located at the base of the spine. It forms the posterior part of the pelvic cavity and serves as a point of attachment for various muscles and ligaments of the pelvic floor.
- Coccyx: The coccyx, commonly known as the tailbone, is a small, curved bone located at the lower end of the sacrum. It provides additional support to the pelvic floor and serves as an attachment site for ligaments and muscles.
- Pelvic Girdle: The pelvic girdle consists of two hip bones, also known as coxal bones or innominate bones. Each hip bone is composed of the ilium, ischium, and pubis, which fuse together during adolescence. The pelvic girdle forms the anterior and lateral aspects of the pelvic cavity.
II. Muscles of the Female Pelvic Floor:
The female pelvic floor contains several layers of muscles that provide support and control to the pelvic organs. These muscles can be divided into three main groups:
- Superficial Muscles: The bulsospongiosus muscle surrounds the vaginal opening and plays a role in clitoral erection and compressing the urethra. The ischiocavernosus muscle runs along the sides of the vaginal opening and helps maintain erection of the clitoris. The external anal sphincter encircles the anal opening and assists in controlling bowel movements.
- Middle Muscles: The levator ani complex is a group of muscles that form the primary support for the pelvic organs. It includes the pubococcygeus, iliococcygeus, and puborectalis muscles. These muscles help maintain continence, support the uterus, bladder, and rectum, and provide stability to the pelvic floor.
- Deep Muscles: The obturator internus is a fan-shaped muscle located on the lateral wall of the pelvis. It helps stabilize the pelvic floor and aids in rotation of the hip joint. The piriformis muscle is a small, deep muscle that runs from the sacrum to the hip joint. It contributes to pelvic floor stability and plays a role in hip rotation. The coccygeus muscle, also known as the ischiococcygeus, spans from the ischial spine to the coccyx. It provides support to the pelvic floor and helps maintain its structural integrity.
III. Nerves of the Female Pelvic Floor:
The innervation of the female pelvic floor involves a complex network of nerves that provide sensory and motor functions. The major nerves associated with the pelvic floor include:
- Pudendal Nerve: The pudendal nerve is a key nerve that supplies the muscles and skin of the external genitalia, perineum, and anal region. It arises from the sacral plexus and passes through the greater sciatic notch before entering the pelvis. The pudendal nerve plays a vital role in controlling the voluntary muscles of the pelvic floor, including the external anal sphincter and the muscles surrounding the vagina and clitoris.
- Pelvic Splanchnic Nerves: The pelvic splanchnic nerves, also known as the pelvic autonomic nerves, originate from the sacral segments of the spinal cord. They carry parasympathetic fibers that regulate various pelvic functions, such as bladder and bowel control, as well as sexual arousal and orgasm. These nerves synapse with ganglia located in the pelvic plexus and provide innervation to the smooth muscles of the pelvic organs.
IV. Blood Supply of the Female Pelvic Floor:
The blood supply to the female pelvic floor is derived from several arteries, ensuring adequate oxygenation and nutrient delivery to the pelvic organs and muscles. The major arteries supplying the pelvic floor include:
- Internal Iliac Arteries: The internal iliac arteries are the main blood vessels responsible for pelvic circulation. They give rise to various branches that supply the pelvic organs, including the uterus, bladder, rectum, and vagina. These branches also provide vascular support to the pelvic floor muscles.
- Superior Gluteal Artery: The superior gluteal artery is another important vessel that contributes to the blood supply of the pelvic floor. It originates from the internal iliac artery and provides vascular support to the gluteal region, including some pelvic floor muscles.
V. Impact of Pelvic Floor Anatomy on Function:
Understanding the anatomy of the female pelvic floor is crucial for comprehending its function and the potential issues that can arise. The muscles, nerves, and blood supply work together to maintain continence, support the pelvic organs, and ensure sexual function. However, disruptions in this intricate system can lead to various pelvic floor dysfunctions, such as urinary or fecal incontinence, pelvic organ prolapse, and sexual dysfunction.
Conclusion:
The female pelvic floor is a remarkable anatomical structure consisting of muscles, nerves, blood vessels, and bones that work in harmony to support the pelvic organs, maintain their function, and ensure overall pelvic floor health. The major muscles, including the superficial, middle, and deep layers, provide support, stability, and control to the pelvic organs, contributing to continence and sexual function. The pudendal nerve and pelvic splanchnic nerves innervate the pelvic floor muscles and play a crucial role in motor control and sensory perception. The blood supply, primarily derived from the internal iliac arteries, ensures proper oxygenation and nutrient delivery to the pelvic organs and muscles.
Understanding the intricate anatomy of the female pelvic floor allows healthcare professionals to diagnose and treat various pelvic floor dysfunctions effectively. By identifying the specific muscles, nerves, or blood vessels involved, targeted interventions can be implemented to restore pelvic floor function and alleviate symptoms.
It is important to recognize that each woman's pelvic floor anatomy and function may vary. Factors such as childbirth, hormonal changes, aging, and lifestyle habits can influence the health and integrity of the pelvic floor. Therefore, a personalized approach to pelvic floor assessment and management is necessary to address individual needs.
In conclusion, the female pelvic floor is a complex structure that consists of muscles, nerves, blood vessels, and bones. Its proper function is vital for continence, pelvic organ support, and sexual well-being. Understanding the anatomy of the pelvic floor provides valuable insights into the potential causes and treatment options for pelvic floor dysfunctions. If you are having any pelvic floor issues, contact us - Pelvic Physiotherapy can help!


